Deep Dive into PrEP and PEP – Queering the Sex-Ed
Swathi SB
Dr Swathi SB is a Primary care & HIV physician and public health professional.
Author: Dr. Swathi SB
Co- Author: Dr. Praneeth Pillala

Multiple effective strategies are accessible to people to prevent acquiring HIV infection. This includes using condoms during sex, avoiding sharing of needles while using drugs, periodic testings for HIV and STIs, having open conversations around sexual health and HIV status, and the more recent approach of pre-exposure prophylaxis (PrEP) and post-exposure prophylaxis (PEP) drugs. PEP and PrEP medications include antiretroviral drugs that act against the virus. Antiretroviral drugs continue to transform people’s lives where persons living with HIV with adequate care are able to lead good quality lives and with a lifespan same as those without the infection. Moreover, the recent policy brief by the WHO reiterated the most important message of Undetectable=Untransmittable (U=U), that there is zero risk of transmission of HIV to sexual partner(s) if the person with HIV is on regular treatment with ART and has undetectable viral load level. Thus, treatment for HIV infection is also one of the major ways to prevent transmission of HIV in the population.
Eshaan, a 23-year-old student couldn’t get sleep as he was worried if he had acquired HIV infection. He had engaged in anal sex the previous evening with a person who he met through a dating app and since he didn’t know the person well, he started to worry now. He had previously heard about post-exposure prophylaxis (PEP) for preventing HIV from a friend but wasn’t sure if he needs to take it and whether he has crossed the time duration within which he can take it. He was feeling very guilty and scared and the information he found on Googling was confusing. He wasn’t able to come to a definite conclusion on what to do. He finally reached out to a friend and discussed the situation.
Like Eshaan, described above, many individuals go through a lot of stress and live with the fear of acquiring HIV, which may result in compromised sex life, pleasure, excessive self-testing due to phobia around it. But understanding the various strategies and the principles that go behind choosing them can help one make informed decisions on what preventive measures seem appropriate to one’s own safety. This article focuses on PEP and PrEP whose use has been growing in India as an important preventive measure for HIV infection, especially among the queer community. Whether taking PrEP or PEP is a good strategy for you to prevent HIV, when should one take PrEP vs PEP and what considerations should one make before starting these are some of the questions that the article will aim to address. One should bear in mind that these multiple preventive strategies briefed above need not be seen as mutually exclusive and many of them can be taken in combination which will also be discussed.
What is PrEP and PEP

PrEP and PEP are both antiretroviral drugs taken to prevent HIV infection. PEP (post-exposure prophylaxis) is a drug regimen taken (in a combination of three or more) in an emergency situation that can be considered risky in terms of acquiring HIV be it sexual exposure, needle prick injuries (occupational or otherwise), or injuries with blood exposure. PEP is a highly effective strategy to prevent acquiring HIV after a possible HIV exposure. This medication should be started as soon as possible considering it an emergency and can be initiated only up to a window of 72 hours post-exposure.
PrEP (Pre-Exposure Prophylaxis) is a two-drug regimen of antiretroviral drugs taken to prevent contracting HIV infection before potential high-risk sexual exposure. Hence PrEP is what is taken in a planned manner. It was approved by the US – FDA in 2012 and by the Drug Controller General of India in 2016. PrEP is known to be highly effective for preventing HIV through sexual exposure when taken as advised but is less effective for sharing needles. Both PEP and PrEP have similar ways of action – the drugs prevent the virus from replicating in the immune cells thus preventing the person from acquiring the infection. The drugs reach a safe concentration in the mucosa and tissue layers of the genital and anal areas, thus acting like a guard at the site of the entry of the virus itself.
Understanding “risk” to see if PEP and PrEP are for you
To decide whether PEP or PrEP would benefit you, understanding what constitutes high risk for potential exposure to HIV becomes key. Your provider will try to assess the risk of the exposure you are involved in order to help you decide on the necessity of PEP. A few considerations to assess the need of PEP when it comes to sexual exposure includes: 1) the kind of sexual activity involved 2) HIV status of the sexual partner(s) and whether they are on ART 3) sexual partner(s) having higher risk of being HIV positive 4) person’s perception of the risk.
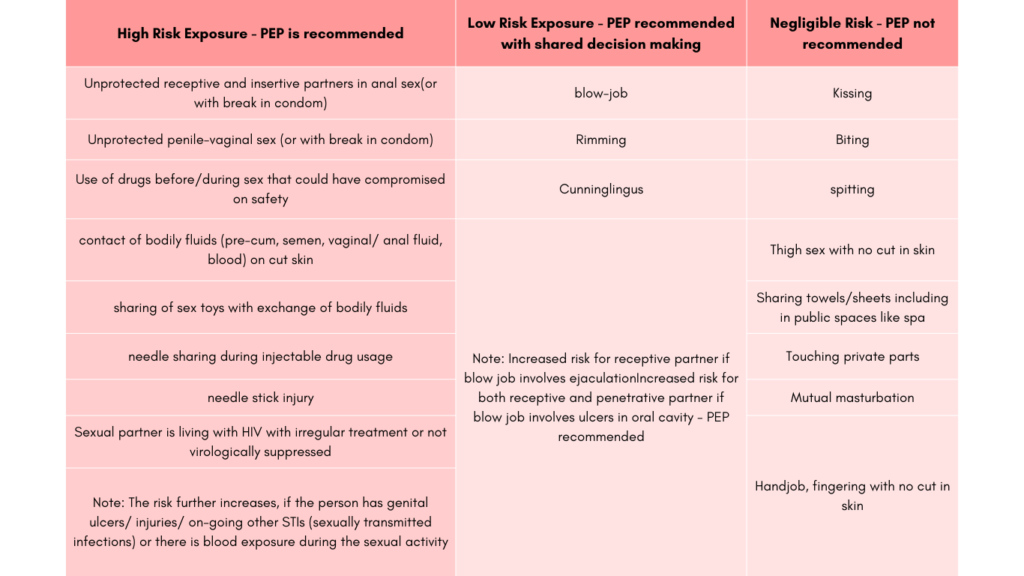
Not all sexual activities pose a high risk for HIV transmission and thus not warrant the use of PEP. The table below lists the various sexual activities in terms of their potential risk for HIV transmission. This guides in considering the use of PEP post-exposure. In situations which can be considered “high-risk”, especially if one doesn’t know the HIV status of the sexual partner, PEP is definitely advised. This scenario changes if the sexual partner is known to be living with HIV and is on appropriate ART with undetectable viral load levels for more than 6 months (U=U), in which case the risk becomes zero for sexual exposure. Hence having an open conversation with the sexual partner(s) before engaging in sex is always a good idea. Through this, one can understand whether the person knows about their HIV and other STIs status, get regular testing done, are on PEP/PrEP, what preventive measures do they take to be safe etc.

Since PrEP is a planned strategy to prevent acquiring HIV, the decision to start on PrEP depends on weighing the pros and cons of taking it. Apart from the understanding of what activity constitutes high risk for potential HIV transmission as described above, there are other considerations to see if one would benefit from PrEP. One will benefit from PrEP if one frequently engages in sexual activity that can be considered as high risk, if the sexual partner(s) are living with HIV but are on irregular treatment or are not virologically suppressed, if there is inconsistency in use of condom in the past 6 months, if one engages in chemsex where drugs are involved and there is a chance of compromise on safety during sex, if one engages in sex work, if one generally engages in sex with a person(s) who’s HIV status might not be known or who has higher risk of living with HIV infection.
Getting started and care
People who are currently taking/ want to take PEP or PrEP can face challenges related to medication availability, cost of medications, lack of provider awareness, stigma/confidentiality concerns at health centres. Hence, once you consider taking PEP or PrEP, finding a reliable source becomes key as this would be a support system to navigate the challenges that might come in the way. Some aspects to keep in mind while gauging the reliability of a source before taking PEP/PrEP are: 1. Whether adequate counselling is provided – this would involve giving enough time and listening to understand your situation properly, giving a chance to consider PrEP, instead of blanket statements like “don’t have sex” or “PrEP has too many side effects” or “don’t take PrEP” etc. 2. Whether they are available and accessible to discuss and follow up for all the concerns you may have once you get started on PEP/PrEP 3. Whether they help you navigate if you need to be physically examined or are they available only over call 4. Whether there is care enough to enquire about you, give you enough information and personalised care as opposed to just profiting from dispensing medications, 5. Is your safety and outcome the primary concern of the provider/organisation? 6. Do they have follow-up mechanisms in place?

The cost of continuing PEP/PrEP is one of the main challenges with usual insurance policies not covering HIV-related services. Costs include blood tests, refilling medications, doctor consultations, and follow-ups. Government centres are not yet providing PrEP and PEP beyond occupational exposure through the National Programme (NACP). However, there are a few NGOs that are reliable and are working to reduce some of these barriers. YRG Care and Safe Zindagi who have partnered with NACO provide preventive services that include online counselling, connecting to local centres, providing testing kits, PrEP, supporting to assess risk etc in various cities across India. Similarly, other NGOs or providers who provide these services in a queer-friendly manner include – The Voluntary Health Services (VHS), Chennai, Dr Mahadevan in Coimbatore, Dr Praneeth Pillala in Bangalore, TAAL+ Integrated Health Centre (IHC) and Community Pharmacy (CP). The medication costs in general have been reducing from past several years as the demand has increased. The MRP for both PrEP and PEP ranges between INR 3000 to 4500 depending on the companies. These are mostly available at private centres, NGOs and online pharmacies at subsidised prices (ranging between INR 750 to 2000) with the most subsidised rates being provided by the NGOs.
What taking PrEP would look like:
PrEP comes in different forms of medicines – oral tablets, injections and gels. At present only tablet form is available in India which are usually a combination of TDF+FTC (Tenofovir+Emtricitabine) or TAF+FTC (Tenofovir alafenamide + emtricitabine). Any people who is HIV negative and has no acute HIV symptoms, above the age of 18 years are eligible to take these medications. Knowing the sexual orientation and preferences of sexual activity of the person helps the provider to decide when to start these medications before sex, because the medications take different duration to reach safe concentration in different body tissues. PrEP medication reaches maximum protection level and starts working for receptive anal sex and vaginal sex at about 7 and 21 days of daily use respectively. Whereas for insertive anal or vaginal sex there is no data available.
There are 2 methods of taking PrEP tablets – daily and event-based PrEP. Daily PrEP is taken one pill, once a day, at the same time irrespective of time/ type of sexual exposure. Event-based PrEP (aka on-demand, episodic) is taken as 2:1:1 in planned sexual exposure with changes in the dosing based on the time of the 1st and the subsequent sexual acts, as described in the table and summarised in the figure below.
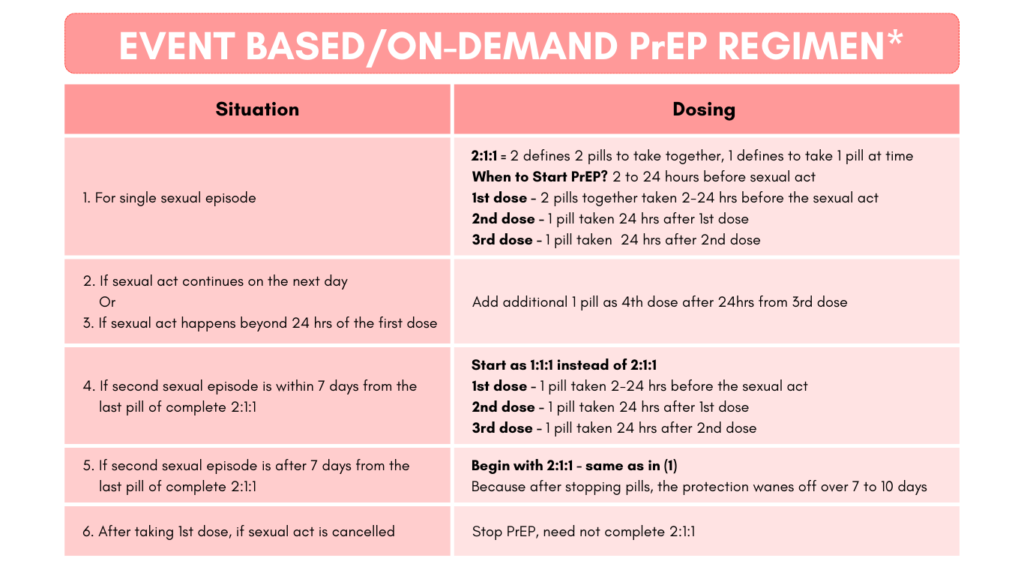
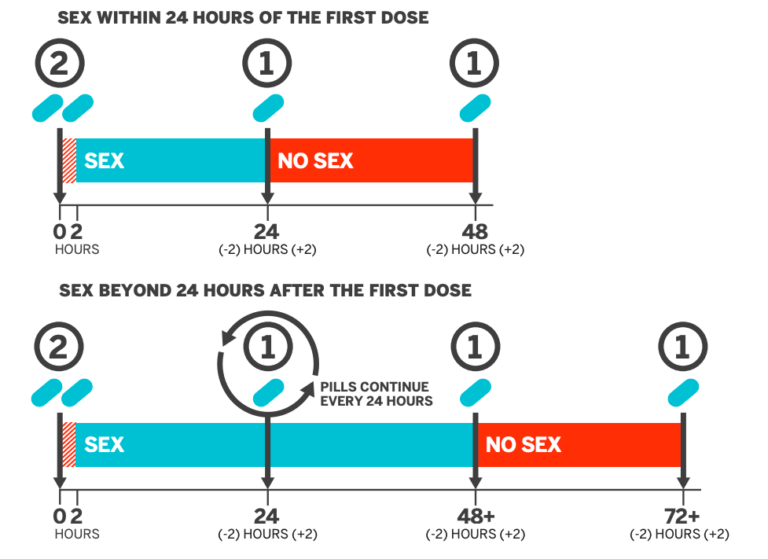
Picture: Dosing of event-based PrEP. Source of the picture: San Francisco AIDS Foundation info sheet
The target level of PrEP medicine concentration in the colorectal tissue reaches 81% and 98% in 2 hrs and 24 hrs after taking 2 pills together respectively. There is a lack of evidence on penile tissue. The benefits of event-based PrEP are the reduction of pill burden and its side effects. People with impaired kidney or liver function tests who cannot tolerate daily PrEP can benefit from this. Event-based PrEP is recommended only for cisgender men, in planned sexual acts with a period of sexual inactivity and who do not want to take daily PrEP. For women and persons with vagina, the tissue bioavailability reduces and the protection is compromised if pills are less than 6 to 7 per week. Hence it is advised to go for daily PrEP and to start 21 days before the sexual act.
Often clinicians are faced with challenges while recommending PrEP for transgender individuals due to lack of recommendations and studies available from India and only a few available from other countries. The challenges to name a few include understanding side effects related to PEP/PrEP, drug-drug interactions with gender-affirming hormone therapy, regular follow-ups by the individual with their doctors, and accessibility of medications. For transgender women especially if taking feminising hormone therapy, daily PrEP is recommended and event-based PrEP is not recommended with the current evidence available. According to the studies, there is no evidence that shows that oral PrEP interacts with gender-affirming hormonal therapy or reduces the effect of either drug. The PrEP medication levels in tissues observed in trans women taking the hormones were slightly lower than that in cis men but this does not affect the efficacy of daily PrEP. Hence, daily PrEP is recommended among trans women. PrEP levels in trans men on hormonal therapy on the other hand do not differ significantly from levels in cis men but, with the current evidence available for AFAB (assigned female at birth) individuals including trans men, daily PrEP is recommended and event-based PrEP is not recommended. The regimen for trans men is a combination of TDF+FTC drugs and not TAF+FTC.
Before starting the medications, your provider will discuss the benefits vs risks of taking PrEP and which regimen would suit you better. A few baseline tests to rule out HIV, hepatitis B, C and and to check your blood parameters will be done. These tests would also be done on follow-up visits. There are certain potential side effects with these medications, such as nausea, diarrhoea, loss of appetite, which resolve in 1 to 4 weeks. More rare side effects include altered kidney/liver functioning and hence will be monitored through the follow-up visits.
What taking PEP would look like:
PEP is most effective if taken within 2 hrs of exposure but can be taken up to 72 hrs post-exposure to potential HIV infection. A few baseline tests to rule out infections just like above will be done but will not be waited for to initiate PEP. The medications generally include a combination of 3 or more drugs and are taken for 28 days. During this period, the person is advised to not engage in sexual activity as that would pose a potential threat to the sexual partner. Follow-up tests would be done upon completion of PEP, at 6 weeks and after 3 months to rule out HIV. PEP is mostly safe but a few may experience headache, nausea, diarrhoea, loss of appetite and if any side effects, these should be discussed with the provider. Upon completion of PEP, you can consider switching to PrEP based on the risk you anticipate in future. While dealing with a high risk exposure, post-exposure prophylaxis needs to be discussed in context of other STIs like Hep B as well.
Considerations while on PEP or PrEP
There are a few aspects to bear in mind while one is on PrEP. PrEP and PEP are generally known to be safe and there are no known drug interactions with gender-affirmative hormone therapy or with oral contraceptives. Thus they can be taken together safely. But if one is on other medications including alternate systems of medicine, it is best to discuss with your provider to make sure that there are no drug interactions that can cause side effects or reduced efficacy of PEP or PrEP. As described above, adequate follow up is key while on PEP or PrEP as this gives an opportunity for one to clarify about other medications, get assessed for side effects, refill medications, get necessary tests done, and discuss other strategies for safe sex in general.
Another important aspect is to be mindful to not miss doses of PEP or PrEP. The drugs need to be in certain concentrations in the blood and genital/rectal tissues for PEP or PrEP to be able to prevent the virus from multiplying. Thus missing the medications can result in inadequate levels of the drugs, thereby reducing the effectiveness of PrEP and PEP. Drug usage including alcohol can affect the regularity of these medications and thus should be used with caution.
While taking PrEP, if you have missed a dose or are on irregular PrEP and have had a high risk exposure, then starting PEP immediately is recommended post exposure (within 72 hrs). Upon completion of 28 days of PEP and testing negative for HIV, you can consider re-starting PrEP after discussion with a trusted provider. If you are unable to take PrEP regularly due to side effects or any other reason, PrEP might not be a good option for you for preventing HIV and thus discontinuation of PrEP can be considered after discussion with your provider. Other preventive strategies will have to be adopted instead.
Discontinuing daily PrEP is always an option when there are changes in your sex life and that you think the risk of getting exposed to HIV has reduced. This shouldn’t be done abruptly though, but continued till 28 days after last potential risk exposure as the protective effect wanes off within 7-10 days of discontinuing medications. HIV testing is recommended after 3 months of discontinuing PrEP.
While PrEP and PEP are effective strategies to prevent acquiring HIV infection, both are not 100% effective. This can be due to the risk of the presence of a virus that is resistant to the medications you are taking as PEP or PrEP. Additionally, PrEP doesn’t prevent you from other STIs. Thus, using condoms is recommended despite being on PrEP and additionally, other strategies like vaccinations for Hep B, HPV etc are to be considered.
Always keeping your needs at the centre and choosing from the various options available that best suits you will take you a long way in terms of safety and better quality of life.
Acknowledgements
We are grateful to Srajan Srivastava for discussing with us various practical questions that need to be addressed in this article. We also thank Vignesh Dhananjayan for recommending some of the reliable sources to access PEP and PrEP. We would extend our gratitude to Shubham Choudhary and Gautam for reviewing the article and providing their valuable feedback.
Resources
- DeHaan E, McGowan JP, Fine SM, et al. PEP to Prevent HIV Infection [Internet]. Baltimore (MD): Johns Hopkins University; 2022 Aug 11. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562734/
- CDC guidelines on PEP and PrEP
- Rutstein SE, Smith DK, Dalal S, Baggaley RC, Cohen MS. Initiation, discontinuation, and restarting HIV pre-exposure prophylaxis: ongoing implementation strategies. Lancet HIV. 2020 Oct;7(10):e721-e730. doi: 10.1016/S2352-3018(20)30203-4. Epub 2020 Aug 27. PMID: 32861269; PMCID: PMC7541752.
- The role of HIV viral suppression in improving individual health and reducing transmission, Policy brief, WHO, 2023 Available from: https://www.who.int/publications/i/item/9789240055179
- Interactions between PrEP and gender-affirming hormone therapy: A research briefing https://www.aidsmap.com/about-hiv/interactions-between-prep-and-gender-affirming-hormone-therapy
- San Francisco AIDS Foundation info sheet:
https://www.sfaf.org/collections/beta/prep-facts-what-are-the-ways-to-take-prep/#slide4
About authors:
Dr. Swathi SB (author) is a Primary care & HIV physician and public health professional. She’s an advocate for health as a right and focuses to address health inequities through research and implementation. She explores the intersection between health, gender, and sexuality and has worked with women in sex work, and transgender communities delivering primary care and understanding the issues related to the provision of comprehensive HIV and primary health care. She’s currently a public health scholar at the Centre of Social Medicine and Community Health, JNU, Delhi.
Dr Praneeth Pillala (Co-Author) is the Co-founder of SarvAveksha – Home based Primary Care, Bangalore,
India. He brings over 8 years of rich and varied clinical, teaching, and leadership experience
including as a Family Physician, senior consultant in HIV/ AIDS with Aging, LGBTQIA+ Health
Care, Sexual & Mental Health, Palliative & Geriatric care. Additionally, he trains medical students,
counsellors and nurses at various health related education institutes to provide compassionate and
comprehensive heath care. Dr. Praneeth has multiple peer reviewed publications and a Co-
investigator in multiple projects. He has won Grand Challenges Canada – Bold Ideas with Big
Impact Award in 2019 for “Empowering Female sex workers including Transgenders to Build Their
Bridges to Healthcare”.
Note: We do not endorse or guarantee the accuracy, completeness, or usefulness of any information provided. Consult your healthcare provider before making any healthcare decisions or changes to your treatment based on information obtained from this platform. In case of a medical emergency or urgent situation, please seek immediate medical attention or contact your local emergency services.
